Endometriosis sufferers tell women in pain to demand better diagnosis
• March 19, 2020

Endometriosis can cause severe dysmenorrhea (period pain) often treated with hot packs. Photo: Brianna Stewart.
Regular excruciating pain and doctor visits was the norm for Stephanie Horrell for 12 years.
Then she was diagnosed with endometriosis.
Stephanie is one of three women spoken to by Te Waha Nui who hope a new report means others will not have to go through the years of torment they have endured.
The document released earlier this month aims to improve the early recognition and management of endometriosis, specifically by empowering primary healthcare professionals to make a suspected diagnosis and commence management.
The condition affects 10% of people with biologically female reproductive systems and causes endometrium, the tissue which lines the inside of the uterus, to grow in places it should not.
Painful periods, bowel problems and pain in other regions of the body are common results.
Kate Simon thinks her life could have been completely different now if her doctor had suggested endometriosis when she first had symptoms.
She was placed on the Combination Oral Contraceptive Pill to manage her painful periods at 14 but feels her doctor did not know enough about endometriosis.
“I definitely had my diagnosis pushed off,” Kate says.
“I was always labelled the mystery case.
“It seemed like no one really cared to find an answer, or if they did it wasn’t in the right direction.”
Kate was diagnosed with chronic fatigue and has recurrent shoulder pain, ultimately caused by endometriosis on her diaphragm, which puzzled specialists.
“It’s hard when everyone wants to have their say but no one wants to take responsibility for diagnosing you.”
This sentiment is echoed by Stephanie Horrell and Madison Randall.
Endometriosis is categorized by four stages. Only stage four can appear on an ultrasound and laparoscopic surgery is required to make a definitive diagnosis.
Stephanie’s diagnosis involved about eight ultrasounds paid out of pocket and numerous misdiagnoses.
The guideline recommends that if symptoms are not controlled or quality of life is not improved by exogenous hormonal therapy after six months, a referral be made to secondary care services.
Stephanie thinks having such a timeline would have made a difference in her life.
“It may have made me doubt myself less, having that validation in your formative years to go forward in your adulthood knowing how to manage it.”
Madison is a medical student and is concerned about the education GPs are getting on the condition.
“I’m just really glad this guide is giving endometriosis some recognition.
“I don’t want to hate on GPs but I have experienced that they won’t talk about it if they aren’t confident or will try steer you in the direction of another diagnosis.
“It pisses me off because how many times are women going to have to stand up and say ‘this is real, I’m not hysterical, this happens and I can feel this. I know this is real’.”
Madison, Stephanie and Kate had to fight for their diagnoses and encourage others to speak up if they feel something is not right.
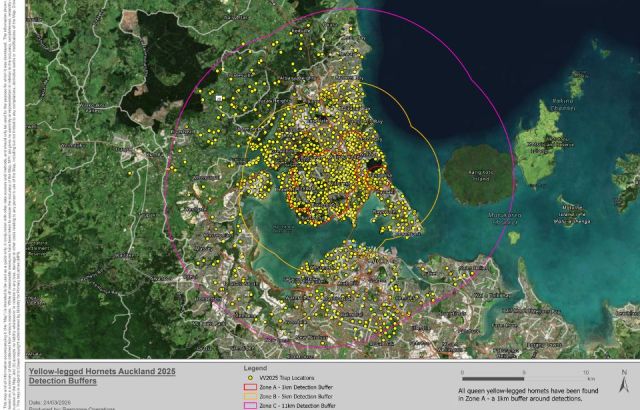
NZ brings in UK experts and AI cameras to tackle yellow-legged hornets on the North Shore
Kieron McVeigh • April 2, 2026

Rhythm unites communities at World of Cultures event in Onehunga
Victoria de Brunner • April 2, 2026

Never been busier: How independent cinema is surviving in Auckland city
Erica O'Neill • April 2, 2026

NZ brings in UK experts and AI cameras to tackle yellow-legged hornets on the North Shore
Kieron McVeigh • April 2, 2026

Rhythm unites communities at World of Cultures event in Onehunga
Victoria de Brunner • April 2, 2026

Never been busier: How independent cinema is surviving in Auckland city
Erica O'Neill • April 2, 2026